Out-of-district hospital trips place strain on families

With a lack of local public health services, Cromwell mother Tammy Dovey's constantly driving to Dunedin for her four-year-old son to see specialists, but the limited use of digital communication and technology has compounded the stress on her family.
Ms Dovey's considered moving to Dunedin to be closer to care – she knows of others who have – and she’s frustrated some appointments that could happen over the phone aren’t – costing her a six-hour return trip.
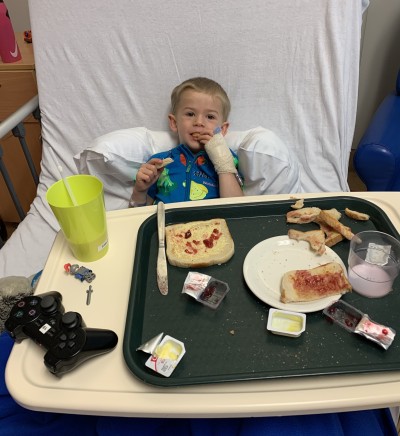
Monty, during a visit to Dunedin Hospital in December.
Funding to help solve this problem was allocated in Labour's 2022 budget - but we're yet to see it all spent. Funding was earmarked for Te Whatu Ora Southern for its digital transformation programme, one goal of which is to allow for more virtual consults to happen.
The project has a four-year timeline, but there are fears the money’s being redirected elsewhere, and recent responses from the new health minister, Ayesha Verrall, to Crux indicate as such.
Queenstown Lakes District mayor Glyn Lewers has recently raised with Crux his concern the bulk of the money will be absorbed in the Dunedin hospital rebuild project, which continues to rack up a high price tag.
Yet, there’s a desperate need for developing digital technologies here in the Central Otago and Queenstown Lakes Districts.
Crux has previously covered how our "rural hospital" - as defined by Te Whatu Ora Southern – is struggling to properly service a growing region, but efforts aren't being made to release the strain on areas where technology could step in.
Since August 2021, Ms Dovey's driven down to Dunedin nine times for appointments for her son Monty, who has Growth Hormone Disorder as well as a more recent diagnosis of Perthese Disease.
A third of these were for "10-minute follow-up appointments, which didn't warrant the six-hour drive", while another two were "proper waste-of-time trips" because the appointment was cancelled with no communication, she says.
Long days of medical appointments in Dunedin are tough on the young family. For emergency treatment in December, they had to rush to the hospital from home for an emergency MRI, finishing up at the hospital 12 hours after they jumped in their car that morning.
Better use of technology would mean less annual leave spent on Dunedin trips, and it would ease the strain on the Dovey family, which also includes Ms Dovey’s husband Ed and eight-year-old son Flint.
"My eldest son (Flint) pulled my heartstrings on the weekend because of the lack of attention. He says 'you never do anything with me' but because I have to take time off work to travel, I haven't got enough annual leave to take time off for him."
Her recent experiences show communication hasn’t gone digital yet either. In January, the family drove to Dunedin for an orthopaedic appointment only to be told on arrival that it had been changed to the following week.
She hadn't received any communication about this - apart from a letter explaining the appointment change, but they'd left for Dunedin before it arrived. Ms Dovey wonders why they didn’t just text, email or call.
“Why are they using the post system to send out appointments when we've got technology these days? Those kinds of aspects, I believe probably need to be looked at.”
When they did return the following Monday, it felt like a waste of time.
“We went back down on the Monday at 6am to get there in time for our appointment – which was at 9.30am – and then we waited for 90 minutes in the waiting room.”
They spoke for seven minutes, and the conversation involved, “we’re just going to wait and see – we’ll see you in three months”, Ms Dovey says.
Frustrated at the unwarranted trip, she vented to the receptionist about the travel time, and is now able to see the specialist involved, Dr John Dunbar, when he travels up to Clyde on outpatient visits - the hospital "hadn't realised" the Dovey family were Cromwell-based.
Similarly, Queenstown local Casey Todd, who has three autoimmune diseases including Hidradenitis Suppurativa, has spent the past ten years being "bounced around the South Island" for healthcare. She explains her condition.
"Basically what happens is I get abscesses under my arms and my chest and my groin overnight. They can appear as big as a tennis ball, down to the size of a marble."
The list of how the medical system has failed her is long, and it does include a lot of unnecessary visits to Invercargill, and a lack of co-ordination between specialists.
It's a tricky situation for Ms Todd – she’s unable to work with her condition and has to live at home with her parents, but she’s expected to travel out of district to receive much of her healthcare - highlighting a lack of services locally.
In the past two years, she's taken six unnecessary trips down to Invercargill, she says, and once there was only a fortnight between two appointments, meaning the expenses add up.
"I pay for my fuel. I pay for everything, because my conditions aren't covered by ACC. I can't get any of that money back.
"When they know I'm coming from out of town, it kind of bugs me that those departments couldn't have gone 'Oh, look, she's coming on this day for dermatology, maybe we could get her for rheumatology at the same time'."
There's safety concerns too, with roads being unsafe in winter and iced over. Ms Todd says she's really grateful she has family support to fall back on, and doesn't know what she'd do without it.
Stories like Ms Todd's and Ms Dovey's, shows the dire for our districts to receive proper health services - and at the least, better use of digital technology to the ease the strain on their wellbeing, annual leave, families and their wallet.
Mayor Glyn Lewers says the district should really see the $155-million worth of funding for the digital transformation project, announced in 2022's budget.

Queenstown Lakes mayor Glyn Lewers expressed fears the money for the programme would go towards Dunedin buildings
His worry: the money for the programme will end up going towards Dunedin Hospital’s new buildings.
But he’ll be watching to make sure Te Whatu Ora Southern’s digital transformation project “actually happens”.
It has a “pretty large budget line” and if it goes ahead it will mean more consults will be able to happen online.
“You can do it virtually - you don't have to travel.”
But responses from the newly-appointed health minister, Ayesha Verrall, suggest the budgeted millions have started being spent in Dunedin firstly.
“The initial work of the programme is focused on the digital requirements for the new Dunedin Hospital buildings.”
Inland Otago residents will need to wait and see what flow-on benefits there are for them, but the minister is positive there will be improvements longer-term locally.
“Digital infrastructure to support virtual consultations is included in the planning for the new Dunedin Hospital. This should benefit our communities by reducing the need to travel to Dunedin for short consultations.”
Te Whatu Ora Southern is also already making use of a telehealth system and has a project manager working to improve uptake this over-the-phone consultation service.
"Our southern team wants to maximise this type of interaction where appropriate to minimise impact on patients around travel and be able to provide care closer to home.”
Ms Dovey says she has an appointment via Teleheath every six months for Monty.
Main image: Tammy Dovey's family with husband Ed (left), Flint (middle) and Monty (right).


























